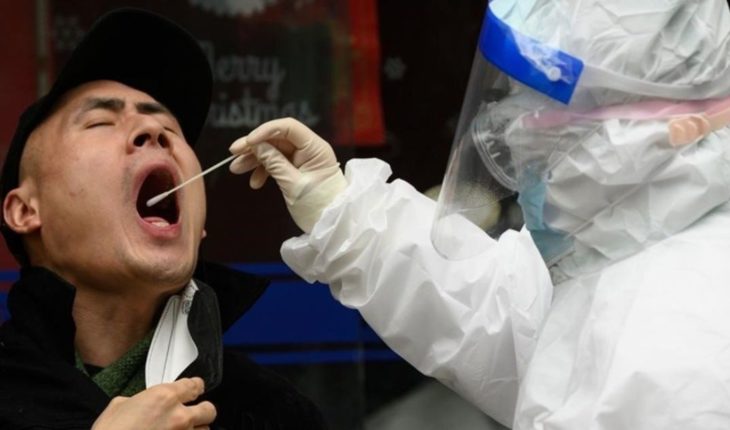
A couple of weeks ago, when the coronavirus pandemic began to slip out of the hands of many Western countries, WHO stressed what countries’ measures should be to control it: social estrangement and “testing, testing and testing.” What’s the point of testing? Basically, for one thing: to make social estrangement more effective. If I know for sure which people carry the virus, I can isolate these people more strictly and thus control their circulation. Also a few weeks ago, in coincidence with that WHO conference, the claim that Argentina has to conduct “massive tests” has been heard, although it is never entirely clear what this would mean. Test the whole country? Test everyone who has symptoms, regardless of what those symptoms are and their travel and contact history? Test all contacts with confirmed cases?
“Testing, testing and testing” was the message given by WHO. Some thought it was about testing without judgment.
The number of tests a country does depends on two things: how the suspicious case is defined (i.e., who should be tested) and the country’s own testing ability, which varies according to, for example, its access to diagnostic kits. Remember that there is no other effective test for the diagnosis that is done by PCR, and that enlisting the laboratories and preparing the staff to be able to operate with the coronavirus is a task that can take some time. Laboratories must not only meet technical and safety conditions but also verify that they are giving the results well: in a pandemic, we cannot afford to have many false negatives (i.e., cases that test negative per laboratory but are actually positive). As for the definition of “suspicious case”, Argentina changed it depending on the progress of the pandemic, as all countries in the world did. Today, from March 30, tested at:Anyone who has a fever and one or more respiratory symptoms (cough, odinophagia, respiratory distress) and in the last 14 days has been in contact with confirmed cases of COVID-19, or has a history of travel outside the country, or has a history of travel or residence in local transmission areas (whether community or conglomerates) of COVID-19 in Argentina.
Every patient with clinical and radiological diagnosis of pneumonia without any other etiology that explains the clinical picture.
Any health personnel who have fever and one or more respiratory symptoms (cough, odinophagia, shortness of breath).
This is exactly the definition of a suspicious case proposed by WHO in its Global surveillance for COVID-19 document caused by human infection with COVID-19, published on 20 March.
Some think that these criteria are too strict and that they were adopted too late, and for that they compare to other countries that managed to control the pandemic, such as South Korea or Germany. The underlying idea would be that Argentina is going to do badly in managing COVID because it is not testing as much as those other countries. Now: Is it reasonable to compare the Argentine situation with that of either of these two countries? Is it true that anyone has done “massive tests”, whatever this means, to stop the spread? Let’s see, Germany
Before we begin, let’s say that among the countries that tested the most per million inhabitant performed is none of the “famous” that are always evoked as an example: are the Faroe Islands, Iceland, Luxembourg, Bahrain and Lichtenstein, among others. What do these countries have in common? Three things: they are small countries, rich and with less than a million inhabitants. This also facilitates at least three things: organization, obtaining sufficient diagnostic kits in a context of global scarcity, and conducting tests on a high percentage of the population.Comparing us with these countries, which have 100 times less population and GDP per capita up to 10 times higher than our own, is really useless. So let’s better compare ourselves to countries that we look a little more like, strongly emphasizing the “a little” part. Germany, for example, quadruples our GDP per capita and has an incomparably superior scientific-technological development to ours: it devotes more than 3% of its GDP to science and technology while Argentina, in 2019, dedicated 0.2% (although it had been promised that it would reach 1.5%). But it doesn’t matter, let’s move forward because something can be learned. It is true that today Germany is one of the countries that has the most tests carried out. By conducting more tests from earlier, the isolation of coronavirus patients was more effective than that of their neighbors, and that is probably one of the causes of their mortality rate being so low, along with the extraordinary health system (which triples, for example, the number of hospital beds in Italy). Now: Did Germany do “mass tests”? Did you test, as some people ask, of anyone with any non-specific symptoms, all contacts of confirmed cases and all those who come from areas of risk? The answer is simple: no. Although he did act very quickly and tested much more than his European peers, largely because he developed very early (on 16 January) his own diagnostic kits and because he already had 85 public and private laboratories ready for the task, it was always tested with a similar criterion to the Argentine. Control of the epidemic in Germany comes following the recommendations of the Robert Koch Institute (RKI), the country’s leading public biomedicine institute. The first case of COVID appeared in Germany in January, and the first measures taken were containment and protection, trying to minimize expansion. The schools, however, remained open and social estrangement was recommended. It was only March 13, when confirmed cases were virtually doubling every other day, schools were closed in some states and two days later, on March 15, borders with neighboring countries were closed. Germany already had 4838 cases and 12 deaths at the time. Total quarantine – with some exceptional permits – was decreed on 22 March, with 18600 confirmed cases and 55 deaths. For reference, in Argentina quarantine was decreed when we had 128 cases and 3 dead. The border closure was on March 16, with 65 cases. Community circulation had not yet been detected, and that is why the definition of suspicious case had not changed. On 25 March, with 31554 cases and 149 dead, Germany changed what would be the equivalent of our definition of suspicious case, i.e. the recommendations made by the RKI on who should be tested. Until that point, the recommendations were that to be tested it was necessary to have been in a risk zone and since then that restriction was removed. That same day, Robert Wieler, the agency’s director, asked laboratories to be strict on the criteria they use to determine who accesses the test, because they are reaching a bottleneck in the production of reagents. He did not ask for further testing but to be tested more rationally and directly, so as not to spend resources in vain.
Robert Wieler of the Robert Kock Institute asks that laboratories be strict with patients being tested.
So said a few days ago Evangelos Kotsoupoulos, the director of Accredited Laboratories in Medicine: “There are only five or six major suppliers of the materials we need worldwide. Germany should focus on who is tested, to ensure that those who have no symptoms but want to know if they have it or not are not tested.” It’s just not possible today to test everyone in a population of our size,” he said in an interview with Die Zeit. And he suggested that the percentage of positive tests on total tests should be higher than it is now, to ensure that tests are not being wasted. South Korea
South Korea is also a developed country, which produces its own diagnostic kits and has a biotechnology industry of the most important worldwide. In addition, he has the experience of the 2015 MERS outbreak, another coronavirus, and thanks to that he has better organized the decentralized testing system. This does not mean that he has tested anyone from the beginning, or that he has had criteria that differ greatly from the Germans or Argentines. He had a completely different tactic to both countries, which was made possible by some very difficult idiosyncratic peculiarities to reproduce. The first case in Korea was confirmed on January 20: what the Korean government did was isolate the person and track all their contacts to isolate them. As of February 19, the number of cases increased in a controlled manner at the rate of about 20 cases per day, indicating that the pandemic was controlled. Between the first case and February 19, during the first month of the pandemic, Korea had conducted 10400 tests, roughly the same as Argentina’s conducted in its first month of coronavirus circulation. However, up to that point he had far fewer cases. If in that first month you tested as much as we did in our first month: How did you control the epidemic? Not, certainly, testing everyone but with a very sophisticated system of monitoring confirmed cases, which consisted of crossing data from those infected with those of the rest of the population to see who they crossed paths with, test them and quarantine them.
Korea combines an aggressive surveillance and tracking system with a large number of tests.
For this, the situation in Korea is privileged for three reasons: It is the country with the highest proportion of debit/credit card expenses in the world.
It is one of the countries with the most teleflyus per person of the world. In fact, he has more phones than people. And movements can be tracked with great precision.
It has unparalleled public surveillance technology. Since 2018, Korea has had more than one million surveillance cameras installed in public places. In 2010, each individual was captured by a camera on average 83 times per day. And the numbers are probably higher now.
Using this technology of monitoring and tracking its inhabitants, Korea did “track and test” and maintained a moderate number of tests until then, because there was no need to test. But if you look at the charts, the number of tests began to scale dramatically thereafter, to get to do more than 11 thousand tests per day today. I mean, today Korea does more tests on a day than it did in its whole first month, what happened then? The number of cases, mostly attributed to a person, which has since become famous as the “patient 31” was fired. This woman attended a massive ceremony of Shincheonji Church in Daeogu, a city of 2 and a half million inhabitants. The Korean government then began to pursue and test all members of the sect, regardless of whether or not they participated in that one-off meeting. It is assumed that, indirectly, this “super transmitter” infected more than a thousand people. Since then, Korea’s strategy had to be scaled and that is why it began to increase the number of tests, although always using the same criterion: contact with confirmed cases verified through surveillance systems. Even today, in Daegu, almost half of cases are concentrated in all of South Korea. Who does the most tests today?
We can continue to compare country by country, but it doesn’t make much sense because the message is: the amount of tests that are done, by itself, does not indicate anything. In a context where the same virus has a mortality rate of less than 1% in some places and more than 10% in others, it is clear that many other variables need to be controlled to make a reasonable diagnosis of the situation and understand where each country is standing. And there are several examples that make this clear. Today, many of the countries that do the most tests are the worst in terms of coronavirus in both the number of infected and the death toll, such as Italy, Spain and the United States.This does not, of course, mean that doing more tests is bad, but that not necessarily doing more tests implies that one is better positioned in the fight against SARS-CoV2. If Italy, the United States and Spain are doing so many tests today, it is not because they have a more lax definition of suspicious case than ours, but simply because the pandemic got out of hand. All three took too long to take containment measures, so their spillover curves got out of control a long time ago, exceeding the capacity of the health system. The United States, which has done almost a million and a half tests, has more than 10,000 deaths: about 30 killed by coronavirus every million inhabitants. Italy, which has already done about 650 thousand tests, has more than 13 thousand dead, 216 every one million inhabitants. Argentina has one dead every million inhabitants.
So with testing anymore, because the amount of tests that are done depends on the time of circulation of the virus. Simply put it: doing 5000 tests when there are 30 new cases a day is a waste, doing 5000 tests when there are 500 thousand new cases per day is insufficient. Each country’s strategy for tackling coronavirus is global and changes according to clinical and epidemiological factors, as WHO itself recommends. It is worth clarifying that WHO rightly discourages the testing of PCR on asymptomatic or mild symptoms patients, except in cases where they have had contact with an individual with COVID-19 confirmed. So comparing the number of tests in a country that had early total quarantine with one that did nothing for months and now has the positive rate doubling every two or three days is nonsense. It doesn’t contribute anything and says nothing about where we’re standing today. Well…where are we standing?
For a few days, Argentina has been multiplying the number of tests it performs per day, thanks to the decentralization and sending of diagnostic kits to more laboratories, and the good news is that, even increasing the number of tests and having expanded the definition of suspicious case, the number of positives per day has not increased significantly and remains in the order of 100.
The chart was shared on Twitter by Rodrigo Quiroga, RESEARCHER at CONICET. Red represents positive cases and blue represents the number of tests.
Although it is a preliminary fact, because of the number of days since the change in definition and the beginning of decentralization, it is encouraging: it means that although – as we know – Community transmission has already begun, it does not seem to be at least as abundant as it imagined, and this is almost certainly due to the mitigating effect of the transmission that the early quarantine decreed by the National Government had.We will have to keep an eye on how the data evolves. , to continue to leave our homes as little as possible and, above all, to maintain measures of social estrangement even when the total quarantine is lifted. By that time, we will surely need to do more tests than are being done now, and for that the laboratories are being prepared and buying the necessary diagnostic kits. In this note: